Sensory Processing Disorder
Sensory processing disorder (SPD) is the inability to use information received through the senses in order to function smoothly in daily life. SPD is not one specific disorder but rather an umbrella term to cover a variety of neurological disabilities. Sensory processing disorder is also called Sensory Integration Dysfunction (SI Dysfunction) and Dysfunction in Sensory Integration (DSI). SPD happens in the central nervous system, at the “head” of which is the brain. When processing is disorderly, the brain cannot do its most important job of organizing sensory messages. The child cannot respond to sensory information to behave in a meaningful, consistent way. He may also have difficulty using sensory information to plan and carry out actions that he needs to do. Thus he may not learn easily. The following infograpic, courtesy of www.sensoryprocessingparentsupport.com summarises many of the more common signs of Sensory Processing Disorder.

SENSORY MODULATION PROBLEMS
The most common category of SPD is Sensory Modulation Disorder. This is suspected when the child exhibits one or more symptoms with frequency, intensity and duration. This chart provides a quick overview of common problems.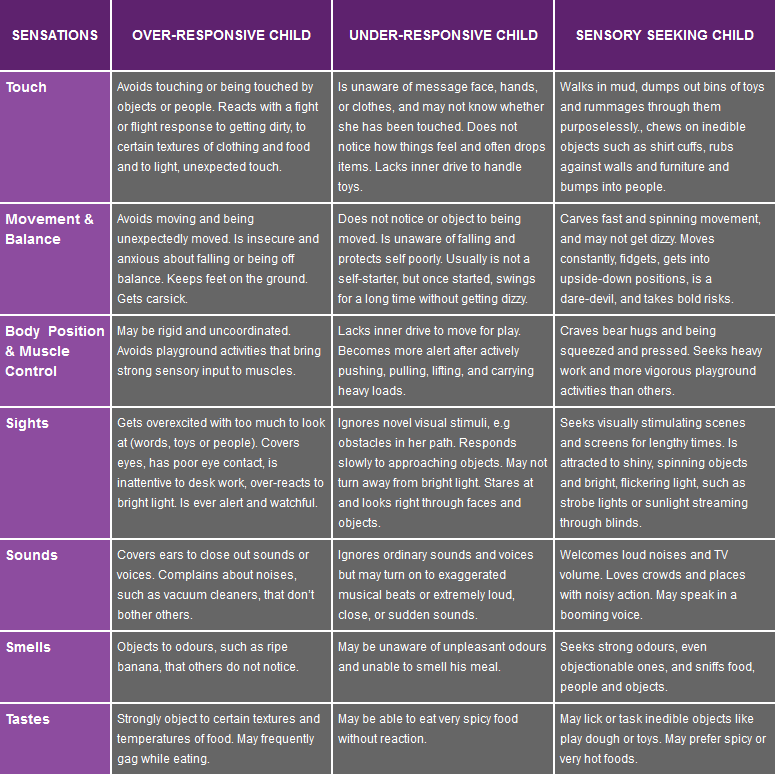
SENSORY DISCRIMINATION PROBLEMS
Another category of SPD is Sensory Discrimination Disorder, which is the difficulty in distinguishing one sensation from another, or in understanding what a sensation means.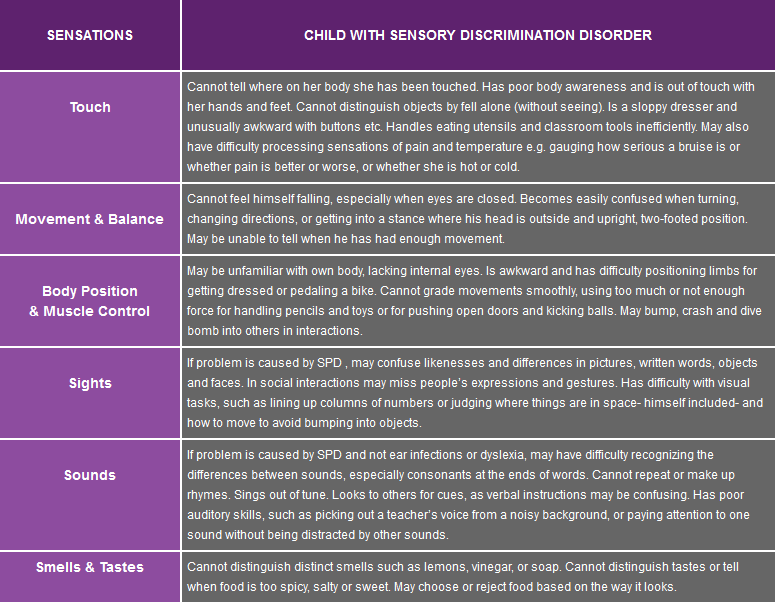
SENSORY-BASED MOTOR PROBLEMS
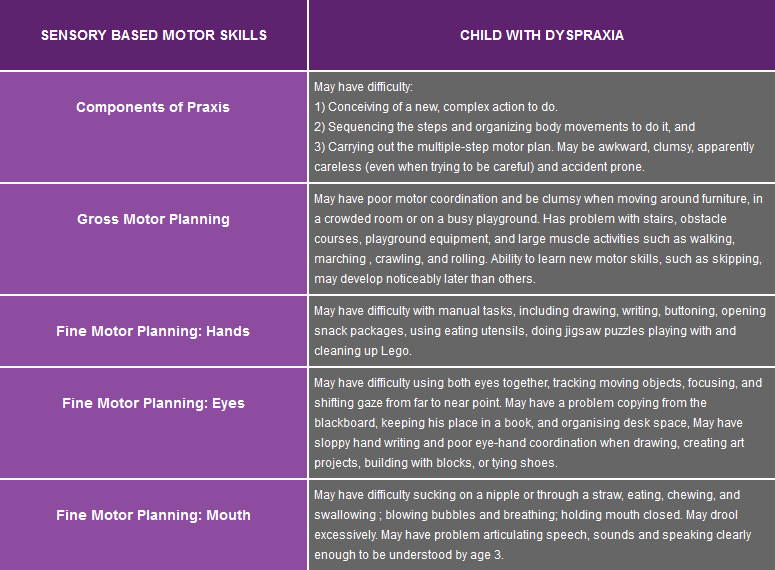
The third category of SPD is Sensory-Based Motor Disorder, which includes two types, Postural Disorder involving problems with movement patterns, balancing and using sides of the body together (bilateral coordination) and Dyspraxia whereby the child has problems performing coordinated and voluntary actions.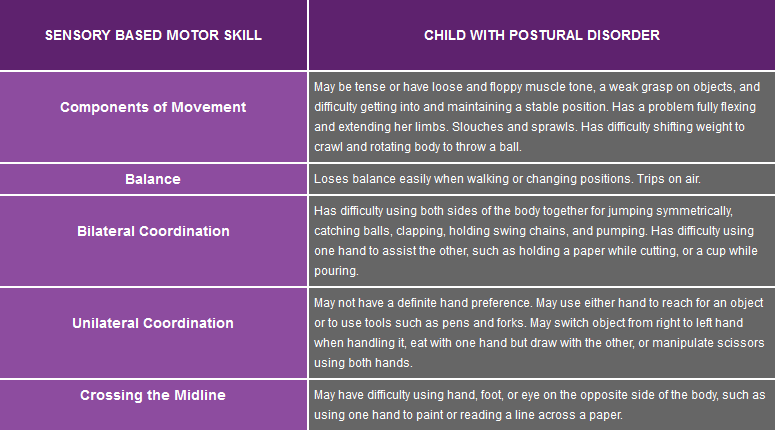
SENSORY MOTOR QUESTIONNAIRE FOR PARENTS
Touch: Does your child…
- Avoid or dislike getting hands messy?
- Become upset when face is washed?
- Become upset when having hair combed or fingernails cut?
- Prefer long-sleeved clothing or jackets, even when it is hot?
- Avoid wearing clothes made of certain fabrics?
- Has trouble changing clothing when seasons change?
- Avoid going barefoot, especially in sand or grass?
- Become irritated by tags or clothing?
- Complain if socks are not on correctly?
- Complain about bumps on bed sheets?
- Seen to crave being held or cuddled?
- Express discomfort when touched in a friendly way by others?
- Prefer to touch other rather than be touched by them?
- Tend to bump or push others?
- Seems excessively ticklish?
- Seem over-sensitive to pain, and be bothered by small cuts?
- Show an unusual need to touch certain textures, surfaces and toys?
- Mouth objects or clothing often?
- Have difficulty judging how much strength to use, e.g petting animals with much force?
Movement: Does your child…
- Become anxious or distressed when feet leave the ground?
- Avoid climbing or jumping?
- Appear reluctant to participate in sports and motor games?
- Seem fearful of catching balls?
- Show fear of falling or heights?
- Dislike elevators or escalators?
- Dislike riding in a car?
- Dislike activities where head is upside down or when lifted overhead?
- Love to be tipped upside down or lifted overhead?
- Seek out all kinds of movement activities?
- Enjoy merry-go rounds and fast rides?
- Jump often and for long time on beds or bouncy surfaces?
- Like to spin himself/herself?
- Rock his/her body of head?
- Bang head on purpose?
- Throw him/herself against floor, wall, or other people for fun?
- Take unusual risks during play?
Visual : Does your child…
- Become easily distracted by visual stimulation?
- Express discomfort at bright lights?
- Avoid or have difficulty with direct eye contact?
- Have a hard time picking out a single object from many, such as finding a specific toy in a toy box?
Auditory: Does your child…
- Become distracted or have a problem when surrounded by a lot of noise?
- Respond negatively to unexpected or loud noises?
- Like to make loud noises?
Taste and Smell: Does your child…
- Explore objects by smelling them?
- Seem bothered by smells that most other people do not notice?
- Chew or lick nonfood items?
SENSORY RELATED SKILLS
Activity Level: Does your child…
- Tend to be especially active or always on the go?
- Tend to fidget excessively in a chair when eating or working?
- Tend to lack carefulness and to be impulsive?
- Seem aggressive in play?
Feeding: Does your child…
- Need assistance to feed himself/herself?
- Tend to eat in a sloppy manner?
- Frequently spill liquids?
- Drool?
- Have trouble chewing?
- Have difficulty swallowing?
- Have difficulty or dislike eating foods with lumps, such as chunky soups?
- Stuff or put too much food in her/her mouth at once?
Organisation: Does your child…
- Frequently lose things, such as homework or coat?
- Get lost easily?
- Have difficulty tolerating changes in plans or expectations?
- Have difficulty changing from one activity to another?
- Need extra assistance to get started with a task or activity?
- Become easily distracted while working or playing?
- Have a short attention span?
Sleeping: Does your child…
- Have irregular sleep patterns?
- Wake frequently during the night?
- Have a difficult time falling asleep?
- Requires less sleep than other children?
Social-emotional: Does your child…
- Have trouble getting along with other children his/her age?
- Seem overly sensitive to criticism?
- Seem overly anxious or fearful?
- Tend to be quiet or withdrawn?
- Tend to be easily frustrated?
- Tend to unusually uncooperative or stubborn?
- Have temper tantrums or outbursts of anger?
- Seem to need more protection from life than other children?
CHARACTERISTICS OF TACTILE DYSFUNCTION
The sensory avoider with over-responsivity (tactile defensiveness) has difficulties with passive touch (being touched).
He may:
- Respond negatively and emotionally to light-touch sensations, exhibiting anxiety, hostility or aggression. He may withdraw from light touch, scratching or rubbing the place that has been touched. As an infant, he may have rejected cuddling as a source of pleasure or calming.
- Respond negatively and emotionally to the possibility of light touch. He may appear irritable or fearful when others are close, as when lining up in the school yard.
- Respond negatively or emotionally when approached from the rear, or when touch is out of his field of vision, such as when someone’s foot grazes his under a blanket or table.
- Show fight or flight response when touched on the face, such as having his face washed.
- Respond negatively when hairs on his body are displaced and rubbed the wrong way. A high wind or even a breeze can raise his hairs, literally ruffling his feathers.
- Become upset in weather with rain or wind.
- Be excessively ticklish.
- Over-responds to physically painful experiences, making a big deal over a minor scrape or splinter.
- Respond similarly to dissimilar touch sensations. A raindrop on his skin may cause as adverse response as a thorn.
- Strongly resist being touched by a barber, dentist, nurse, or doctor
- Exhibit behaviour that seems stubborn, rigid, inflexible, willful, verbally or physically pushy, or other wise difficult for no apparent reason, when it is actually an aversive response to tactile stimuli.
- Rebuff friendly or affectionate pats or caresses, especially if the person touching is not a parent or familiar person.
- Be distracted, inattentive, and fidgety when quiet concentration is expected.
- Prefer receiving a hug to a kiss. He may crave the deep pressure of a hug, but try to rub off the irritating light touch of a kiss.
- Resist having fingernails or toenails trimmed.
- Dislike surprises.
- Resist brushing his teeth.
- Be a picky eater, preferring certain textures such as crispy or mushy foods. The child may dislike foods with unpredictable lumps, such as tomato sauce or vegetable soup as well as sticky foods like rick or cake icing.
- Refuse to eat hot or cold food.
- Avoid giving kisses.
- Resists baths, or insist that bath water be extremely hot or cold.
- Curl or protect hands to avoid touch sensations.
- Be unusually fastidious, hurrying to wash a tiny bit of dirt off his hands.
- Avoid walking barefoot on grass or sand, or wading in water.
- Walk on tiptoe to minimize contact with the ground.
- Fuss about clothing , such as stiff new clothes, rough textiles, shirt colors, turtlenecks, belts, elasticized waists, hats and scarves.
- Fuss about footwear, particularly sock seams. He may complain about shoe laces.
- Prefer short sleeves and shorts and refuse to wear hats and mittens in winter.
- Prefer long sleeves and pants and insist on wearing hats and mittens in summer.
- Avoid touching certain textures or surfaces, like some fabrics, blankets, rugs or stuffed animals.
- Need to touch repeatedly certain surfaces and textures that provide soothing and comforting tactile experiences, such as a favourite blanket.
- Withdraw from art, science, music, and physical activities to avoid touch sensations.
- Avoid messy play, such as sand, finger paint, paste, glue, mud and clay, perhaps becoming tearful at the idea.
- Stand still or move against the traffic in group activities such as obstacle courses or movement games, keeping constant visual tabs on others.
- Treat pets roughly, or avoid physical contact with pets.
- Arm himself at all times with a stick, toy, rope, or other handheld weapon.
- Rationalize verbally, in socially acceptable terms why he avoids touch sensations e.g. My mother told me not to get my hands dirty.
- Withdraw from a group or resist playing at other children’s homes.
- Have trouble forming warm attachments with others. Experiencing difficulty in social situations, he may be a loner, with a few close friends.
The sensory disregarder with under-responsivity may show atypical responses to passive and active touch.
The child may:
- Not notice touch unless it is very intense.
- Be unaware of messiness on his face, especially around his mouth and nose, not noticing a runny nose.
- Be unaware of messed hair or sand in his hair.
- Not notice that clothes are in disarray, or that cuffs or socks are wet.
- Not notice heat, cold, or changes in temperature indoors or out often keeping on a jacket even when sweating, or not reaching for a jacket even when shivering.
- Show little or no response to pain from scrapes, bruises, cuts or shots, perhaps shrugging off a broken finger or collarbone.
- When barefoot, not complain about sharp gravel, hot sand, or stubbed toes.
- Not react to spicy, peppery, acidic, hot or mouth burning food or crave this kind of food.
- Be oblivious to weather conditions with wind or rain.
- Fail to realise that he has dropped something.
- Not move away when leaned on or crowded.
- Appear to lack inner drive to touch, handle or explore toys and materials that appeal to most other children.
- Require intense tactile stimulation to become engaged in the world around him, but not actively seek it.
- Hurt other children or pets during play, seemingly without remorse but actually not comprehending that pain that others feel.
The sensory craver with sensory seeking needs extra touch stimuli, both passive and active.
The child may:
- Ask for tickles or back rubs.
- Enjoy vibration or movement that provides strong sensory feedback.
- Need to touch and feel everything in sight.
- Rub certain textures over her arms and legs to get light touch input.
- Rub or bite his own skin excessively.
- Constantly twirl hair in fingers.
- Frequently remove socks and shoes.
- Seem compelled to touch or walk barefoot on certain surfaces and textures that other people find uncomfortable or painful.
- Seek certain messy experiences, often for long duration.
- Seek very hot or cold room temperature or bath water.
- Have high tolerance for sweltering summer or freezing winter weather.
- Dive into food often cramming mouth with food.
- Prefer steaming hot , icey cold, extra-spicy, or excessively sweet foods.
- Use his mouth to investigate objects, even after the age of two.
- Show in your face behaviour, getting very close to others and touching them, even if his touches are unwelcome.
The child having a problem with tactile discrimination may:
- Poor body awareness and not know where his body parts are or how they relate to one another.
- Be unable to identify which body parts have been touched without looking.
- Have trouble orienting his arms, legs, hands, and feet to get dressed.
- Be unable to identify familiar objects solely through touch, needing the additional help of vision.
- Be unable to know the difference between similar items he is using such as a crayon versus a marker.
- Be disheveled, with shoes on wrong feet, socks sagging, shoelaces untied, waistband twisted, and shirt un-tucked.
- Avoid initiating tactile experiences, such as picking up toys, materials, and tools that are attractive to others.
- Have trouble perceiving the physical properties of objects, such as their texture, shape, size, temperature or density.
- Be fearful in the dark.
- Prefer standing to sitting, in order to ensure visual control of his surroundings.
- Act silly in the classroom.
- Have a limited imagination.
- Have a limited vocabulary because of inexperience with touch sensations.
The child with dyspraxia may:
- Have trouble conceiving of, organizing, and performing activities that involve a sequence of movements, such as cutting, pasting, colouring, assembling collage pieces or recipe ingredients, applying nail polish.
- Have poor gross motor control for running, climbing and jumping.
- Have poor eye-hand coordination.
- Require visual cues to perform certain motor tasks that other children can do without looking, such as zipping, snapping , buttoning and unbuttoning clothes.
- Put on gloves or socks in unusual ways.
- Have poor fine-motor control of his fingers for precise manual tasks e.g. holding and using eating utensils and classroom tools, such as crayons, stapler, scissors and hold punchers.
- Struggle with handwriting, drawing, completing worksheets, and similar tasks.
- Have poor fine-motor control of his toes for walking barefoot or in flip-flops.
- Have poor fine-motor control of his mouth muscles for sucking, swallowing, chewing or speaking.
- Be a messy eater.
- Have poor self-help skills and not be a self-starter.
THE VESTIBULAR SENSE
The vestibular system tells us about up and down and whether we are upright or not. It tells us where our heads and bodies are in relation to the earth’s surface. It sends sensory messages about balance and movement from the neck, eyes and body to the central nervous system for processing and then helps generate muscle tone so we can move smoothly and efficiently. It tells us about whether we are moving or standing still and whether objects are moving or motionless in relation to our body in addition to informing us what direction we are going in and how fast. The vestibular system gives us information necessary for many everyday skills such as gravitational security, movement and balance, muscle tone, bilateral co-ordination, motor planning, vision and hearing and emotional security.
CHARACTERISTICS OF VESTIBULAR DYSFUNCTION
The over-responsive child who shows intolerance for movement may:
- Dislike playground activities such as swinging, spinning and sliding.
- Be cautious, slow moving, and sedentary, hesitating to take risks.
- Seem willful and uncooperative.
- Be very uncomfortable in lifts and on escalators.
- Demand continual physical support from a trusted adult
The child with gravitational insecurity may:
- Have a great fear of falling, even where no real danger exists.
- Be fearful of heights, even slightly raised surfaces.
- Become anxious when her feet leave the ground, feeling that even the smallest movement will throw her into outer space.
- Be fearful of climbing, or descending stairs, and hold tightly to the banister.
- Feel threatened when her head is inverted, upside down or tilted e.g. when having her hair shampooed over the sink.
- Be fearful when someone moves her .
- For self-protection, try to manipulate her environment or other people.
- Have poor proprioception and poor visual discrimination
The sensory disregarder with under-responsiveness to vestibular sensations may:
- Not notice or object to being moved.
- Seem to lace inner drive to move actively.
- Once started, swing for a lengthy time without getting dizzy.
- Not notice sensation of falling and may not respond efficiently to protect himself by extending his hands or a foot to catch himself
The sensory-seeking child with increased tolerance for movement may:
- Need to keep movement, as much as possible, in order to function.
- The child may have trouble sitting still or staying in a seat.
- Repeatedly, vigorously shake her head, rock back and forth and jump up and down.
- Crave intense movement experiences, such as bounding on furniture, using a rocking chair, turning in a swivel chair or assuming upside-down positions.
- Be a thrill seeker, enjoying fast-moving or spinning playground equipment or seeking the fast and scary rides at an amusement park.
- Not get dizzy, even after twirling or spinning rapidly for a lengthy amount of time.
- Enjoy swinging very high or for long periods of time.
- Like seesaws or trampolines.
The sensory child with sensory-based postural disorder affection movement of the head, balance, muscle tone and bilateral coordination may:
- Lose her balance unless both feet are firmly planted, as when stretching on tiptoes or standing on both feet when her eyes are closed.
- Easily lose her balance when out of a two-footed position, e.g climbing stairs, riding a bicycle, hopping or standing on one foot.
- Move in an uncoordinated, awkward way.
- Be fidgety and clumsy.
- Have a loose and floppy body.
- Feel limp when you lift her, move her limbs to help her get dressed or try to help her balance.
- Ten to slump or sprawl in a chair or over a table.
- Prefer to lie down rather than sit upright.
- Find it hard to hold up her head, arms and legs simultaneously when lying on her stomach.
- Sit on the floor with her legs in a”W” position.
- Have difficulty turning doorknobs or handles that require pressure, and have a loose grasp on pencils, scissors or spoons.
- Have a tight, tense grasp on objects to compensate for looseness.
- Have problems with digestion and elimination, such as frequent constipation or poor bladder control.
- Fatigue easily during physical activities.
- Be unable to catch herself from falling.
- Not have crawled as a baby.
- Have poor body awareness.
- Have poor gross motor skills and frequently stumble and trip.
- Be clumsy at sports or active games.
- Have poor fine motor skills and difficulty using pencils, crayons or combs.
- Have difficulty making both feet or both hands work together such as jumping up and down or throwing and catching a ball.
- Have difficulty using one foot of hand to assist the other during tasks e.g standing on one foot to kick a ball.
- Have trouble using both hands in a smooth, alternating manner.
- Not have an established hand preference by the age or four or five.
- Avoid crossing the midline.
- Have a hard time with organization and structured activities.
The sensory child with dyspraxia or poor motor planning may:
- Have difficulty conceptualizing, organizing and carrying out a sequence of unfamiliar movements.
- Be unable to generalize what she has already learned in order to accomplish a new task.
The child who is emotionally insecure may:
- Get easily frustrated and give up quickly.
- Be reluctant to try new activities.
- Have a low tolerance for potentially stressful situations.
- Have low self esteem.
- Be irritable in others company and avoid or withdraw from people.
- Have difficulty making friends or relating to peers.
THE PROPRIOCEPTIVE SENSE
Proprioception tells us about our own movement and body position. Proprioception informs us:
- Where our body or body parts are in space.
- How our body parts relate to one another.
- How much and how quickly our muscles are stretching.
- How fast our body is moving through space.
- How our timing is.
- How much force our muscles put forth.
Proprioception dysfunction is the inefficient processing of sensations perceived through the muscles and skin, as well as the joints. The child with poor proprioception has difficulty interpreting sensations about the position and movement of his body parts. He may show confusion when walking down a street, getting in and out of the bath or crossing the playground. He may be clumsy and easily frustrated. He may exert too much pressure or too little pressure on objects, struggling to turn door knobs and regularly breaking toys and pencils. He may have a poor grip on forks or combs and experience difficulty zipping a jacket, buttoning a shirt or getting out of bed in the dark.
CHARACTERISTICS OF PROPRIOCEPTIVE DYSFUNCTION
The child who is over-responsive to proprioceptive input may:
- Prefer not to move.
- Become upset when limbs are passively moved.
- Become upset when it is necessary to stretch or contract his muscles.
- Avoid weight-bearing activities such as jumping, hopping, running, crawling or rolling.
- Be a picky eater
The under-responsive child may:
- Have low tone.
- Fix elbow to ribs when writing, or knees tightly together when standing to compensate for low muscle tone.
- Break toys easily.
The sensory seeking child may:
- Deliberately bump and crash into objects in the environment.
- Stamp or slap his feet on ground with walking.
- Kick his heels against the floor ro chair.
- Bang a stick or other object on a wall or fence while walking.
- Engage in self-stimulatory activities such as head banging, nail biting, finger sucking or knuckle cracking.
- Like to be tightly swaddled in a blanket or tucked in tightly at bedtime.
- Prefer shoelaces, hood and belts to be tightly fastened.
- Chew constantly on objects.
- Appear to be aggressive
The child with poor discrimination and dyspraxia may:
- Have poor body awareness and motor control.
- Have difficulty planning and executing movement.
- Have difficulty positioning his body when someone is helping him into his coat or when he is trying to dress or undress.
- Have difficulty knowing where his body is in relation to objects and people frequently falling, tripping or bumping into obstacles.
- Show fear when moving in space.
The child with emotional insecurity may:
- Avoid participation in ordinary movement experiences because they make him feel uncomfortable or inadequate.
- Become rigid, sticking to the activities that he has mastered and resisting new physical challenges.
- Lack self-confidence.
- Become timid in unfamiliar situation.
THE VISUAL SENSE
Children with visual sense dysfunction are inefficient in coordinating visual discrimination and visual-motor skills with vestibular, proprioceptive and postural mechanisms eg. Their eyes and bodies are out of syn. When dysfunction involves movement (ie tripping on air), posture (slumping at the desk) and body awareness (difficulty learning left and right) it is likely that the problem is sensory based.
CHARACTERISTICS OF VISUAL DYSFUNCTION
The child with a problem with basic visual skills may:
- Have headaches, eye strain, or red, burning, itchy or teary eyes.
- Rub eyes or blink, frown and squint excessively.
- Complain about blurred images when looking at pictures, print or faces.
- Complain of seeing double.
- Complain that words seem to move on the page.
- Turn or tilt her head as she reads across the page.
- Hold a book too closely or lower her face too closely to the desk.
- Have difficulty seeing the black board in school.
- Have difficulty shifting her gaze from one objet to another e.g looking from the black board to her copybook.
- Have difficulty focusing on stationary objects.
- Frequently loses her place on the page, reread words or lines and omit numbers, letters, words or lines when reading or writing or need to use her finger to keep her place.
- Have difficulty tracking or following a moving object, such as a ping pong ball.
- Fatigue easily during schoolwork or sports-related activities.
The child with difficulty modulating visual sensations may:
- Shield her eyes to screen out sights, close or cover one eye or squint.
- Avoid bright lights and sunlight.
- Be uncomfortable or overwhelmed by moving objects or people.
- Duck or try to avoid objects coming toward her, such as a ball or another child.
- Withdraw from classroom participation and avoid group movement activities.
- Avoid direct eye contact.
- Experience headaches, nausea, dizziness when using eyes.
- Be unaware of light/dark contrast, edges and reflections.
- Be unaware of movement, often bumping into moving objects such as swings.
- Respond late to visual information, such as obstacles in her path.
- Seek bright lights, strobe lights and direct sunlight.
- Seek visual stimulation, such as finger flicking, spinning and peering at patterns.
- Move excessively during visual tasks such as workbook activities.
The child with poor visual discrimination may:
- Have difficulty seeing objects in three dimensions.
- Seem overwhelmed by moving objects or people.
- Have difficulty judging relative distances between objects such as letters, words, numbers or drawings on a page; between oneself and objects in the environment.
- Not understand concepts such as up/down, forward/back, before/after and first/second.
- Have difficulty stringing beads together in order, following a pattern to build with blocks.
- Have difficulty in team sports that require awareness of position on the field.
- Confuse likenesses and differences in pictures, words, symbols and objects and have difficulty distinguishing properties of objects.
- Repeatedly confuse similar beginnings and endings of words e.g tree/three, fight/flight/fright.
- Have difficulty with schoolwork involving the size of letter, the spacing of words and letters on the line and the lining up of numbers. The child may revers letters e.g b/d.
- Have difficulty differentiating objects in the foreground and background, necessary to distinguish one word on a page, or a face in a crowd.
- Be unable to form mental images of objects, people or scenarios to envision what she reads or hears, or relate pictures and words to the “real thing”.
- Have difficulty describing thoughts and actions both verbally and in writing.
- Be a poor speller.
- Have difficulty remembering what he did or saw during the day.
- Be unable to interpret how objects would feel, just by looking at them; the child must touch the kitten to know that it is soft and furry.
- Fail to comprehend what she is reading, or quickly lose interest.
- Have a short attention span for reading or copying information from the black board and have a poor visual memory of what she read
The child with poor visual-motor skills may:
- Have poor eye-hand coordination.
- Be unable to use her eyes to guide hand movement necessary for accurate orientation of drawings and words on a page. She may be unable to stay within the lines when she colours and her.
- Writing may be crooked and poorly spaced.
- Have difficulty with fine-motor tasks involving spatial relationships, such as doing jigsaw puzzles, rearranging dollhouse furniture and cutting along lines.
- Have poor eye-foot coordination and difficulty walking upstairs or kicking balls.
- Have poor gross-motor skills and difficulty moving on playground equipment, such as reaching for and climbing on monkey bars.
- Avoid sports and group activities in which movement is required.
- Have difficulty with rhythmic activities.
- Have poor coordination and balance.
- Have difficulty sound out a word silently and then saying it.
- Orient drawings poorly on the page, or write uphill or downhill.
- Have exceedingly poor posture while at the table or desk or twist in an unusal way to see the teacher or a book.
- Withdraw from classroom participation.
- Have low self-esteem.
THE AUDITORY SENSE
The vestibular and auditory systems work together as they process sensations of movement and sound. Hearing is the ability to receive sound and this basic skill develops in the womb. The ear’s influence on physical development is profound as it is vital not only for hearing, balance and flexibility but also for bilateral coordination, respiration, speaking, self-esteem, social relationships, vision and academic learning.
CHARACTERISTICS OF THE AUDITORY SENSE
The child with difficulty modulating auditory sensations may:
- Be distressed by loud noises, including the sound of voices.
- Be distressed by sudden noises, such as thunder, fire alarms, sirens and balloons popping.
- Be distressed by tinny or metallic sounds.
- Be distressed by high-pitched sounds such as whistles, violins and sopranos.
- Be distressed by sounds that do not bother others such as a toilet flushing, a distant church bell or soft background music.
The child with poor auditory discrimination may:
- Seem unaware of the source of sounds or may look all around to locate where they come from.
- Have difficulty recognizing particular sounds, such as voices or cars coming down the street.
- Have difficulty tracking a sound in the environment, such as footsteps.
- Have difficulty recalling, repeating or referring to words, phrases, conversations, song lyrics or instructions both right away or later.
- Be unable to focus or maintain attention to a voice, conversation, story or sound without being distracted by other sounds.
- Have difficulty hearing or reading jokes, verbal math problems, crossword puzzle definitions or discussions and understanding how all the information fits together into a coherent whole.
- Have a poor sense of timing and rhythm when clapping, marching, singing, jumping rope or playing band instruments.
The child with receptive language difficulty may:
- Have a problem discriminating similar sounding word sounds, especially consonants at ends of words, as in cap/cat, bad/bag, side/sign.
- Have a short attention span for listening to stories or for reading.
- Misinterpret questions and requests.
- Be able to follow only one or two instructions in sequence.
- Look to others before responding.
- Frequently ask for repetition, or be less likely than others to ask for clarification of ambiguous directions or descriptions.
- Have difficulty recognizing thymes.
- Have difficulty learning new languages.
The child with expressive language difficulty may:
- Have been a late talker.
- Have difficulty putting thoughts into spoken or written words.
- Talk off topic.
- Have difficulty closing circles of communication.
- Have difficulty correcting or revising what she has said so others can understand.
- Have a weak vocabulary.
- Use immature sentence structure.
- Have poor spelling skills.
- Have a limited imagination in fantasy play.
- Have difficulty making up rhymes.
- Sing out of tune.
- Have difficulty with reading, especially out loud.
- Require more time than other children to respond to sounds and voices.
The child with speech and articulation difficulty may:
- Be unable to speak clearly enough to be understand.
- Have a flat, monotonous voice quality.
- Speak very loudly or very softly.
- Speak with a hoarse, husky, strident, weak, or breathy voice.
- Speak hesitantly or without fluency and rhythm.
INTEROCEPTION
Interoception is a sense that allows us to notic einternal body signals like a growling stomach, racing heart, tense muscles or full bladder. Our brain uses these sigals as clues to our emotions. Research shows that the ability to clearly notice body signals is linked to the ability to identify and manage the following emotions and more:
Hunger
Tiredness
Focus
Fullness/Thirst
Need for Bathroom
Calm
Pain
Anger
Boredom
Anxiety
Sadness
Body Temperature
Distraction
Differences in Interoception are very common and can lead to challenges in identifying exactly how one feels. Common signs of interoception differences can include difficulty with one or more of the following:
- Recognizing when hungry, full or thirsty
- Toilet training (daytime and/or night time)
- Identifying when sleepy
- Overly sensitive or not sensitive enough to pain
- Pinpointing symptoms of illness
- Identifying emotions in self
- Identifying emotions in others
- Recognizing building signs of distress (before a full meltdown)
- Independently using coping strategies during times of distress
DIAGNOSING THE PROBLEM
What should you do and where should you start?
- You can take the “wait and see” approach and wait to see if the dysfunction improves over time.
- You can improve your child’s “sensory diet” by liaising with your child’s teacher to develop a home and school sensory program that will help strengthen your child’s skills.
- Seek specialist evaluation to screen your child for possible risk factors or do a full Sensory Profile evaluation.
Therapies
- To reduce tactile defensiveness.
- To improve tactile discrimination.
- To develop better body awareness and improve postural security.
- To improve balance.
- To improve bilateral coordination.
- To improve motor planning.
- To improve fine motor skills.
- To improve extension against the pull of gravity.
- To improve flexion.
- To reduce gravitational insecurity.
- To improve ocular control and visual discrimination.
- Physical Therapy
- Speech and Language Therapy
- Visual Therapy
- Auditory Training
- Chiropractic
- Craniosacral Therapy
- Hippotherapy
- Martial Arts
- Nutritional Therapy
- Perceptual Motor Therapy
- Psychotherapy
Sensory diet
A balanced sensory diet is a planned and scheduled activity program that a therapist develops to meet the needs of a specific child’s nervous system. Its purpose is to help the child become better regulated and more focused, adaptable and skillful. A sensory diet fulfills the physical and emotional needs of the child and it includes a combination of alerting, organizing and calming activities.
Alerting activities benefit the under-responsive child and include:
- Crunching dry cereal, popcorn, crisps, nuts, crackers, pretzels, carrots, celery, apples and ice-cubes.
- Taking a shower.
- Bouncing a therapy ball or beach ball.
- Jumping up and down on a trampoline.
Organising activities help regulate the child’s responses and include:
- Chewing granola bars, fruit bars, licorice, dried apricots, chees, gum, bagels or bread crusts.
- Hanging by the hands from a chinning bar.
- Pushing or pulling heavy loads.
- Getting into an upside down position.
Calming activities help the child decrease sensory over-responsivity or over stimulation and include:
- Sucking a soother, hard candy, frozen fruit bar or spoonful of peanut butter.
- Pushing against walls with hands, shoulders, back, buttocks and head.
- Rocking, swaying or swinging slowly to and fro.
- Cuddling or back rubbing.
- Taking a bath.
Activities for development
Activities to develop the tactile system
Activities to develop the vestibular system
Activities to develop the proprioceptive system
Activities to develop the auditory system
Activities to develop the visual system
Activities to develop fine-motor skills
Activities to develop motor-planning skills
Activities to develop bilateral coordination
Suggestions to develop self-help skills
Dressing
Snack & meal time
Chores
Bathing
Sleeping
Promoting the childs success at school
Recognise and document those activities that lead to sensory overload.
Reduce sensory overload.
For tactile defensive children help him find a place in the classroom that reduces the likelihood of contact with other children.
Allow the tactile defensive child to occupy last place in “The Line” so that he can control the space between him and the child in front of him.
For children with visual discrimination eliminate clutter on bulletin boards.
Secure artwork on the walls so they don’t flutter.
Remove swaying mobiles from the ceiling.
Adjust window blinds to prevent sunshine from flickering through.
Allow the child to sit near the front of the class to avoid the distraction of moving children.
White space around each written math problem helps the child focus on one problem at a time.
Cover classroom hard surfaces such as desktops, tiles and painted walls to reduce the reflection of noise which can distract the child with auditory processing problems.
Ensure that the child is not seated near a humming fish tank or fluorescent bulb or a window.
Playing classical music such as Bach and Mozart while the children are working softens the auditory environment.
Keep animals, pain supplies and other aromas that might affect the child with olfactory processing disorder away from the child’s desk.
Ensure that suitable furniture is available for the child who frequently falls off his chair because of inefficient body awareness.
Place tennis balls under the legs of the chair to stabilize it.
For older children who are expected to remain seated for long periods of time ensure that a comfortable cushion is provided.
For fidget preschoolers, a ball to sit on may be preferred over a chair.
Keep chalkboards and worksheet clean as fuzzy lines present problems for children with visual processing disorder.
Plan transitions from one task to another by ensuring that the child is aware in plenty of time.
Plan movement breaks between and during activities for the fidgety child.
Devise team efforts and reward systems for team endeavours.
Encourage the child to be an active rather than a passive learner.
Give the child time to process questions and formulate answers.
Simplify instructions.
Break down assignments into small chunks.
Provide a choice of writing implements.
Respect the child’s needs.
Anticipate problems and provide alternatives to such situations.
Adapting your own behaviour
GLOSSARY OF SENSORY PROCESSING TERMS
Academic Learning: The development of conceptual skills, such as learning to read words and multiply numbers, and to apply what one learns today to what one learned yesterday.
Accommodation: The basic visual skill of focusing on objects at varying distances.
Active Touch: Using one’s hands, feet and mouth to gather tactile information about objects in the environment.
Activity Level: The degree of one’s mental, emotional or physical arousal. Activity level can be high, low or in between.
Acuity: The keep perception of a sight, sound or other sensation.
Adaptive Behaviour: The ability to respond actively and purposefully to changing circumstances and new sensory experiences.
Amygdala: The brain structure that processes small sensations and produces memories with an emotional component.
Arousal: A state of the nervous system ranging from sleep to awake, from low to high. The optimal state of arousal is the “just right” midpoint between boredom and anxiety, where we feel alert and calm.
Articulation: The production of speech sounds.
Attention-Deficit/Hyperactivity Disorder: An umbrella term for a problem interfering with one’s ability to attend to and stay focused on meaningful tasks, control one’s impulses, and regulate one’s activity level. The main symptoms of this neurologically based disorder are hyperactivity, in attention and or impulsivity.
Audition: The ability to receive and apprehend sounds: hearing.
Auditory Discrimination: The ability to receive, identify, differentiate, understand and respond to sounds.
Auditory Training: A method of sound stimulation designed to improve a person’s listening and communicative skills, learning capabilities, motor coordination, body awareness and self-esteem.
Aversive Response: A feeling of revulsion and repugnance toward a sensation, accompanied by an intense desire to avoid or turn away from it.
Basic Visual Skills: Unconscious mechanisms of sight.
Behaviour: Whatever one does, through actions, feelings, perceptions, thoughts, words or movements in response to stimulation.
Bilateral Coordination: The ability to use both sides of the body together in a smooth and simultaneous manner.
Bilateral Integration: The neurological process of integrating sensations from both body sides: the foundation for bilateral coordination.
Body Awareness, body percept or body scheme: The mental picture of one’s own body parts, where they are, how they interrelate and how they move.
Body Position: The placement of one’s head, limbs and trunk. Proprioception is the sense of body position.
Compressed Visual Attention: Focusing on just one object at a time rather than seeing the whole picture.
Crossing the Midline: Using a hand, foot or eye on the opposite side of the body.
Defensive System: The component of a sensory system that alerts one to real or potential danger and causes a self- protective response. This system is innate.
Developmental Delay: The acquisition of specific skills after the expected age.
Discrimination System: The component of a sensory system that allows one to distinguish differences among and between stimuli. This system is not innate but develops with time and practice.
Dyspraxia: Difficulty in conceptualizing, motor planning , sequencing and carrying out unfamiliar actions in a skillful manner.
Early Intervention: Treatment or therapy to prevent problems or to improve a young child’s health and development.
Emotional Security: The sense that one is loveable and loved, that other people are trustworthy, and that one has the competence to function effectively in everyday life.
Evaluation: The use of assessment tools, such as tests and observations, to measure a person’s developmental level and individual skills or to identify a possible difficulty.
Expressive Language: The spoken or written words and phrases that one produces to communicate feelings and thoughts to others.
Extension: The pull of the muscles away from the front of the body; straightening or stretching.
External Senses: The senses of touch, small, taste, vision and hearing.
Exteroception: Referring to the five external senses.
Eye-hand Coordination: The efficient teamwork of the eyes and hands, necessary for activities such as playing with toys, dressing and writing.
Eye-Motor Skills: Movements of muscles in the eyes.
Far Senses: The external and environmental senses of vision and hearing.
Fine-Motor: Referring to movement of the small muscles in the fingers, toes, eyes and tongue.
Fixing: Pressing one’s elbows into one’s side or one’s knees together for more stability.
Flexion: Movement of the muscles around a joint to pull a body part toward its front or centre; bending.
Fluctuating Responsivity: A combination of over-responsivity and under-responsivity as the child’s brain rapidly shifts back and forth.
Gravitational Insecurity: Extreme fear and anxiety that one will fall when one’s head position changes or when moving through space, resulting from poor vestibular and proprioception processing.
Gross Motor: Referring to movement of large muscles in the arms, legs and trunk.
Gustatory Sense: The sense of perceiving flavor : taste.
Habituation: The neurological process of tuning out familiar sensations.
Hidden Senses: Internal senses.
Hyperactivity: Excessive mobility, motor function, or activity such as fingertapping, jumping from one’s seat or constantly moving some part of the body ; fidgetiness.
Increased Tolerance For Movement: Underresponsivity to typical amounts of movement stimulation; often characterized by craving for intense movement experiences such as rocking and spinning.
Inhibition: The neurological process that checks one’s overreaction to sensations.
Inner Drive: Every person’s self-motivation to participate actively in experiences that promote sensory processing.
Integration: The combination of may parts into a unified, harmonious whole.
Internal Eyes: Body awareness.
Internal Senses: The subconscious senses that regulate bodily functions, such as heart rate, hunger and arousal including the interoceptive, vestibular and proprioceptive senses.
Interoception: The body-centered sense involving both the conscious awareness and the unconscious regulation of bodily processes of the heart, liver, stomach and other internal organs.
Intersensory Integration: The convergence of sensations of touch, body position, movement, sight, sound and smell.
Intolerance to Movement: The over-reactivity to moving or being moved rapidly, often characterized by extreme distress when spinning or by avoidance of movement through space.
Lateralization: The process of establishing preference of one side of the brain for directing skilled motor function on the opposite side of the body, while the opposite body side is used for stabilization: necessary for hand preference and crossing the midline.
Linear Movement: A motion in which one moves in a line, from front to back, side to side, or up and down.
Meltdown: The process, usually caused by excessive sensory stimulation, of becoming “undone” or “unglued,” accompanied by screaming, writhing and deep sobbing.
Midline: A median line dividing the two halves of the body.
Modulation: The brain’s ability to regulate and organize the degree, intensity, and nature of the person’s response to sensory input in a graded and adaptive manner.
Motor Control: The ability to regulate and monitor the motions of one’s muscles for coordinated movement.
Motor Coordination: The ability of several muscles or muscle groups to work together harmoniously to perform movements.
Motor Planning: The ability to organize and sequence the steps of an unfamiliar and complex body movement in a coordinated matter; a piece of praxis.
Muscle Tone: The degree of tension normally present when one’s muscles are relaxed, or in a resting state: a function of the vestibular system, enabling the person to maintain body position.
Olfactory Sense: The far sense that perceives odour : smell.
Oral Apraxia: A sensory-based motor problem affecting the ability to produce and sequence sounds necessary for speech.
Oral Defensiveness: Over-responsivity in the mouth to certain food textures or tastes.
Oral-Motor Skills: Movements or muscles in the mouth, lips, tongue and jaw including sucking, biting, crunching, chewing and licking.
Over-reactivity and Under-reactivity: Exaggerated neurological and physiological processes that we cannot observe and that may cause and over and under responsive behaviour.
Over-Responsivity: Observable behaviour involving a quick or intense response to sensory stimuli that others usually perceive as benign: characterized by exaggerated, negative and emotional responses or withdrawal.
Passive Movement: The act of being moved by something or someone.
Passive Touch: The act of being touched by something or someone without initiating it.
Perception: The meaning that the brain gives to sensory input.
Pervasive Developmental Disorder: Severe, overall impairment in the ability to regulate sensory experiences, affecting the child’s affect and behaviour, interaction with others, and communication skills: similar to, but milder than autism.
Postural Disorder: Difficulty with moving or stabilizing the body to meet the demands of the environment or a particular motor task.
Postural Stability: The feeling of security and self-confidence when moving in space, based on one’s body awareness.
Praxis: The ability to interact successful with the physical environment: to ideate, plan, organize and carry out a sequence of unfamiliar actions; to do what one needs and wants to do.
Proprioceptive Sense: The unconscious awareness of sensations coming from one’s muscles and joints that provides information about when and how muscles contract or stretch; when and how joints bend, extend or are pulled; and where each part of the body is and how it is moving.
Protective Extension: Thrusting out an arm or leg to protect oneself while falling.
Receptive Language: The ability to understand how words express ideas and feelings; language that one takes in by listening and reading.
Regulatory Disorder: A problem with adapting to changing conditions, such as self-calming when distressed; falling asleep and waking up; eating, digesting and eliminating; paying attention; participating socially; and processing sensations.
Self-Regulation: The ability to control one’s activity level and state of alertness, as well as one’s emotional, mental or physical responses to sensations; self-organisation.
Sensitisation: The process of interpreting stimuli as important, unfamiliar, or harmful, even if the stimuli are unimportant, familiar and benign.
Sensory-Based Motor Disorder: A problem with movement such as Postural Disorder and Dyspraxia, resulting from inefficient sensory processing.
Sensory Defensiveness: The tendency to respond to certain harmless sensations as if they were dangerous and painful.
Sensory Diet: The multi-sensory experiences that one normally seeks on a daily basis to satisfy one’s sensory appetite; a planned and scheduled activity program that an occupational therapist develops to help a person become more self-regulated.
Sensory Discrimination Disorder: problems in discerning the characteristics of sensory stimuli and the differences among and between stimuli.
Sensory Integration: The part of sensory processing disorder whereby sensations from one or more sensory systems connect in the brain.
Sensory Integration Treatment: A technique of occupational therapy, which provides playful, meaningful activities that enhance an individual’s sensory intake and lead to more adaptive functioning in daily life. The emphasis is on improving sensory-motor processing rather than on skill training.
Sensory Modulation Disorder: The inability to regulate and orgaise the degree, intensity and nature of responses to sensory input in a graded and adaptive manner.
Sensory-Motor: Pertaining to the brain-behaviour process of taking in sensory messages and reacting with a physical response.
Sensory Processing Disorder: Difficulty in the way the brain takes in, organizes and uses sensory information, causing a person to have problems interacting effectively in the everyday environment. Sensory stimulation may cause difficulty in one’s movement, emotions, attention, relationships, or adaptive responses.
Sensory Seeking: The constant quest for excessive sensory stimulation.
Sequencing: Putting movements, sounds, sights, objects, thoughts, letters and numbers in consecutive order according to time and space.
Sleep Regulation Problem: An irregular pattern of sleeping, such as difficulty falling asleep or sleeping through the night, or the need for an unusual amount of sleep.
Somatosensory: Referring to tactile-proprioceptive discrimination of touch sensations and body positioning; body sensing.
Stimulus: Something that activates a sensory receptor and produces a response.
Tactile Defensiveness: The tendency to react negatively and emotionally to unexpected, light-touch sensations ; a common type of sensory modulation dysfunction.
Tactile Discrimination: The awareness of touching or of being touched b something; the ability to distinguish differences in touch sensations; and the awareness of the physical attributes of an object such as its size, shape, temperature, density and texture.
Tactile-Proprioceptive: Referring to simultaneous sensations of touch and body position.
Tactile Sense: The sensory system that receives sensations of pressure, vibration, movement, temperature, and pain, primarily through receptors in the skin and hair. Protective receptors respond to light or unexpected touch and help a person avoid bodily harm; discriminative receptors provide information about the tactile qualities of the object or person being touched.
Touch Pressure: The tactile stimulus that causes receptors in the skin to respond. Deep pressure such as a hug activates receptors in the discriminative system. Light touch such as a kiss activates receptors in the protective system.
Under-Responsivity: Under-sensitivity to sensory stimuli, characterized by a tendency either to crave intense sensations or to withdraw and be difficult to engage; a subtype of sensory modulation disorder.
Unilateral Coordination: Smooth, independent use of one side of the body, necessary for writing and handling tools.
Vestibular System: The sensory system that responds to the pull of gravity, providing information about the head’s position in relation to the surface of the earth, and coordinating movements of the eyes, head, and body that affect equilibrium, muscle tone, vision, hearing and emotional security. Receptors are in the inner ear.
Vestibular-Proprioceptive: Referring to simultaneous sensations of the head and body positions when one moves.
Vision: The process of identifying sights, understanding what the eyes see and preparing for a response.
Vision Therapy: Treatment to help a person improve visual skills and to prevent learning-related visual problems.
Visual Discrimination: The ability to perceived and interpret sensory information received through the eyes and body as one interacts with the environment and moves one’s body through space.
Visual-Sensory Integration: Combing sights with touch, movement and other sensory messages.
Visual-Motor Skills: Ones movements based on the discrimination of visual information eg eye-hand coordination, eye-foot coordination and eye-ear coordination.
ONLINE RESOURCES.
